We often talk about how pathology has changed over the years but there are also changes happening in the field today. Digital pathology continues to make the news as more labs explore its possibilities, so what is it and how does it benefit patients?
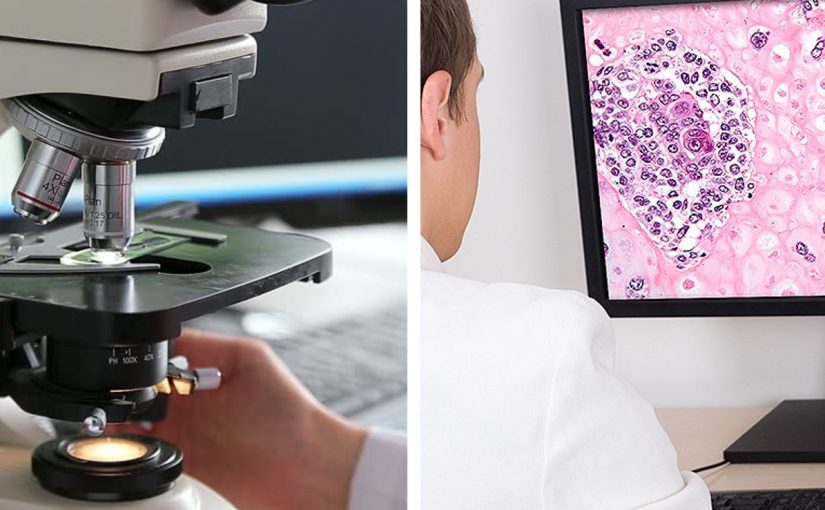
In anatomical pathology, digital microscopy is the conversion of glass microscope slides into image files called “digital slides” using a high-quality scanning machine – the pathology equivalent to computer-based x-rays.
Once digitised, the slide images can be used by the pathologist as an alternative to conventional microscopy for histological (tissue-based) diagnosis. They can also be analysed by computer algorithms to automate the counting of cells highlighted by special stains.
With digital slides, pathologists can directly access image files and view the same case at the same time – from anywhere in the world. This means additional opinions can be readily obtained without the need to ship fragile glass slides from site to site. In complex cases, multiple care teams can collaborate across sites without the delays involved in transporting materials, and this can potentially improve the efficiency of diagnosis and treatment planning. The technology can be particularly beneficial to pathologists operating in remote and isolated environments.
Digitised slides are being increasingly used as teaching aids for medical students and pathology trainees, for quality assurance purposes, and even for examination purposes, ensuring all candidates have access to exactly the same slide images.
Currently the storage of glass slides is a major logistic burden for laboratories, as labs in Australia are required to keep slides for a minimum of 10 years for adults (or until age 25 for children). The ability to review a case is necessary in case a disease recurs. In future, it is possible that retention of high quality digital images may be a substitute for the storage of glass slides.
Finally, the digitisation of clinical data creates new opportunities. Using digital microscopy to count and analyse cells has been shown to be at least as accurate as manual counting by a pathologist and can potentially save time. Computer files can be analysed, shared, archived and compared in ways physical slides cannot. This means larger data sets and potentially new insights provided by emerging technology, which may not have been possible with glass slides.
So are the machines taking over? Not quite. Digital microscopy does not remove the necessity for a highly skilled pathologist to oversee the analysis of slides and interpret accompanying data, particularly in complex cases. It does, however, take some of the manual labour and logistic complexity out of the process – meaning pathology professionals can focus on what really counts – a quick, accurate diagnosis for their patient.
The potential benefits of digital pathology are obvious, but they are difficult to monetise. This is maybe the biggest barrier for anatomical pathology labs considering going digital. The investment in new equipment and training needs to be justified – and without hard numbers, that can be difficult. But as the pathology sector is put under increasing pressure to produce more results in shorter time frames, more and more Australian laboratories are making the leap.