The Newborn Screening test (NBS), also known as the ‘Guthrie’ or ‘heel prick’ test, has been around since 1962, and will be familiar to most parents.
It’s the test where blood is drawn from a baby’s heel, usually within 48-72 hours of birth, and is used to test for cystic fibrosis, hypothyroidism, phenylketonuria, and a host of other conditions.
It was one of those ‘other’ medical conditions that Julie Gravina – mother of twins Charlize and Isaac – had to confront when NBS test results came back indicating something was wrong and that further testing was required.
‘The twins were in a comatose state in the first few days,’ said Julie. ‘We had a range of blood and urine tests to see what was wrong and by day 7 they were diagnosed with a genetic metabolic disorder called propionic acidaemia.’
Propionic acidaemia is a rare inherited condition affecting less than 1 in 100,000 people. Those with propionic acidaemia are unable to process protein components properly, which can lead to abnormal levels of ammonia and acids in the body.
‘We got the newborn screen test results on Friday and were immediately called into The Children’s Hospital at Westmead where they began work straight away to get the ammonia levels down. If we got the results on Monday, they would have died.’
Subsequent specialised biochemical genetic and molecular genetic tests revealed the medical outlook for the twins was poor, necessitating a decision on whether the twins should be booked in as soon as possible for liver transplants.
It was a tough decision but ultimately one taken out of Julie’s hands by the severe nature of the condition.
‘Brain damage can happen at any time. By 9 months of age, Isaac had developed brain damage. He was registered by 12 months and at 19 months had received a transplant,’ said Julie.
Unfortunately, Isaac developed complications post-transplant that he was unable to recover from and passed away at 21 months of age.
After much painstaking consideration, Julie and husband Paul decided to register Charlize for a liver transplant.
‘It was incredibly difficult to make those decisions, but if we hadn’t opted for liver transplants, the prognosis was not good.’
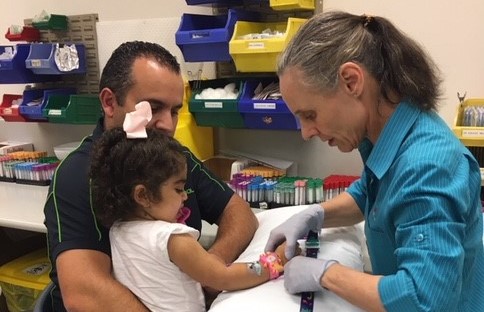
Charlize requires continual monitoring through pathology tests to make sure her amino acids and ammonia levels are at the right levels.
‘Propionic acidaemia is an extremely tough condition to manage. Too little protein and they don’t grow and develop normally, too much and organs start to fail,’ said Clinical Associate Professor Carolyn Ellaway of the NSW Genetic Metabolic Disorders Service, Sydney Children’s Hospital Network and University of Sydney.
‘Brain damage can occur extremely quickly. Charlize needs constant monitoring which she gets through specialised pathology tests.
‘This shows how important pathology is to the healthcare system, helping diagnose conditions and flagging them for immediate attention, and then helping the clinical team to work out appropriate treatments and monitoring progress.’
Charlize has now had two liver transplants, the second one in early 2018.
Thanks to advances in technology and genetic research, the medical conditions the NBS test searches for – including metabolic conditions like propionic acidaemia – continues to grow.
After the introduction of Tandem mass spectrometry by the NSW Health Department in 1997, the NBS test was able to screen for another 30 metabolic disorders. Last year, congenital adrenal hyperplasia was added to the list.